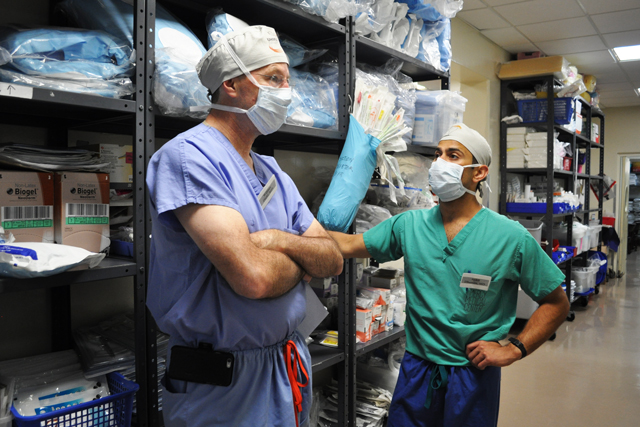
In October 2023, UHMLA embarked on yet another remarkable journey, with passion and dedication to change lives and help people in need. This time, our devoted team members gathered their essential supplies and hit the road for Yantalo, in Peruvian Amazon Jungle—an outreach destination significantly challenging not only for UHMLA but also for any other mission groups.
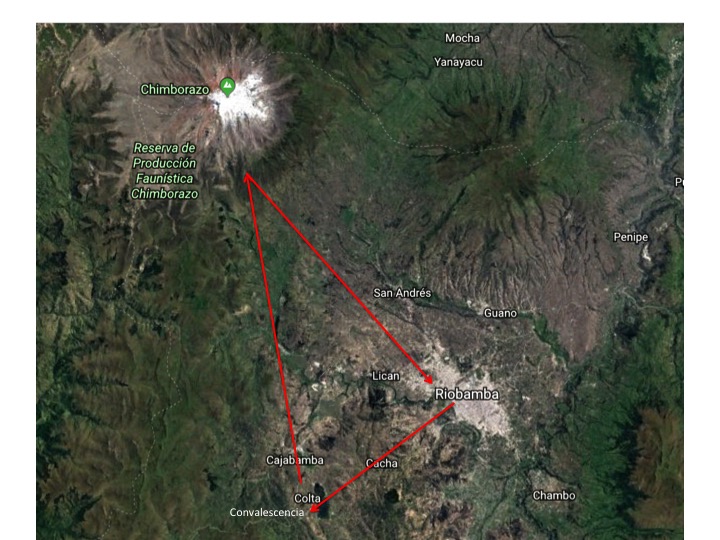
The journey to Moyobamba, the team's lodging destination, is an arduous 24-hour endeavor involving multiple vessel changes. Plus, the team has to travel daily in a small bus along a bumpy road for half an hour to reach the Yantalo Clinic, where crucial surgeries take place.
Yantalo Adelina Soplin Clinic serves the people of the region all year around, it is managed by the Yantalo Peru Foundation with the support of international and Peruvian volunteers. The Clinic was started in 2005 by Dr. Luiz Vasquez inspired by his mother Adelina Soplin’s memory and designed by the volunteers of the New School of Architecture and Design in San Diego, CA. UHMLA is one of the organizations who play a vital impact on the sustainability of the clinic.
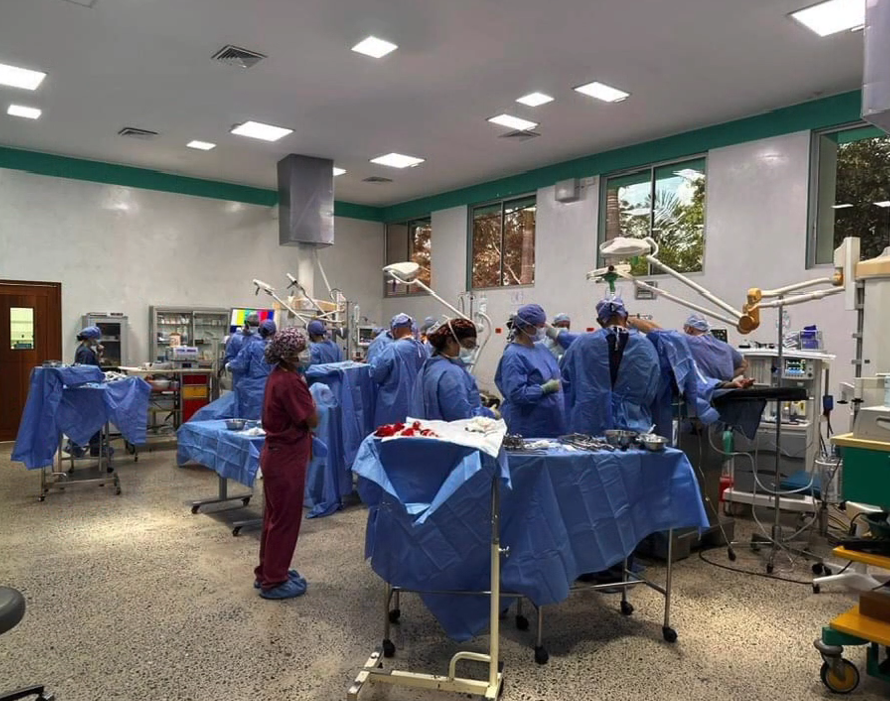
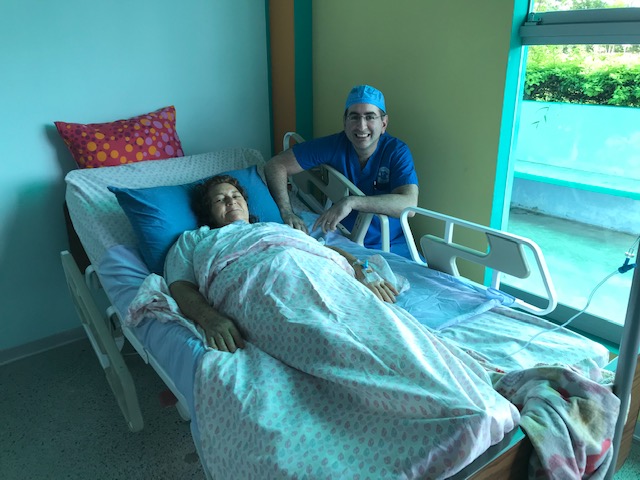
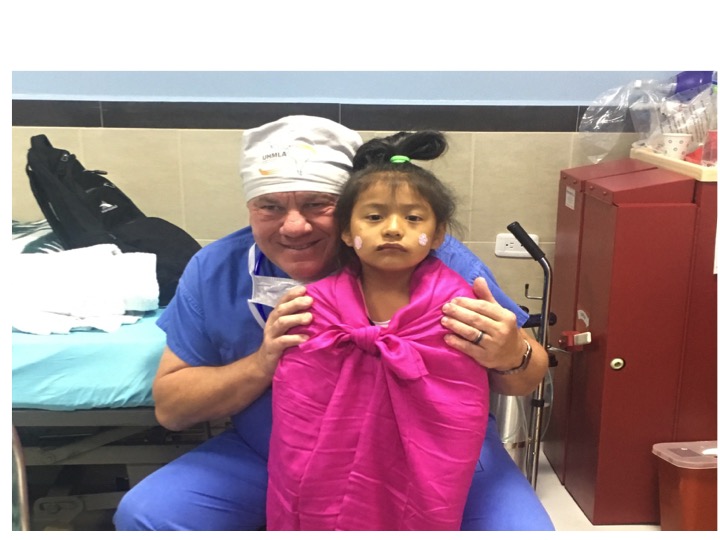
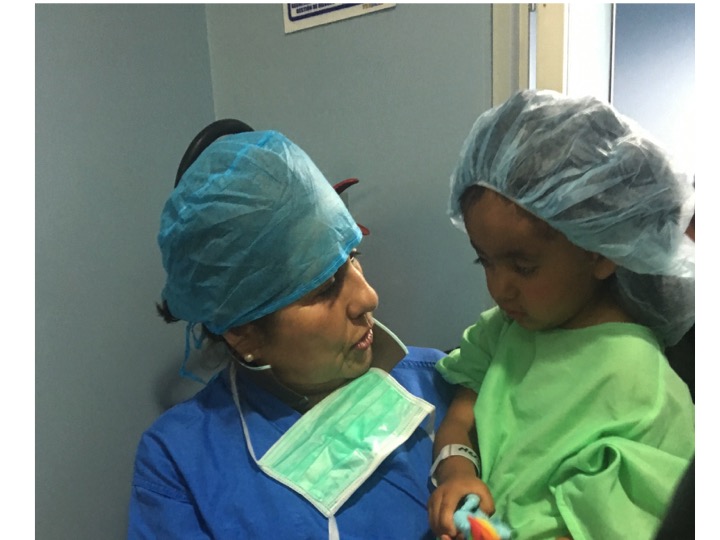
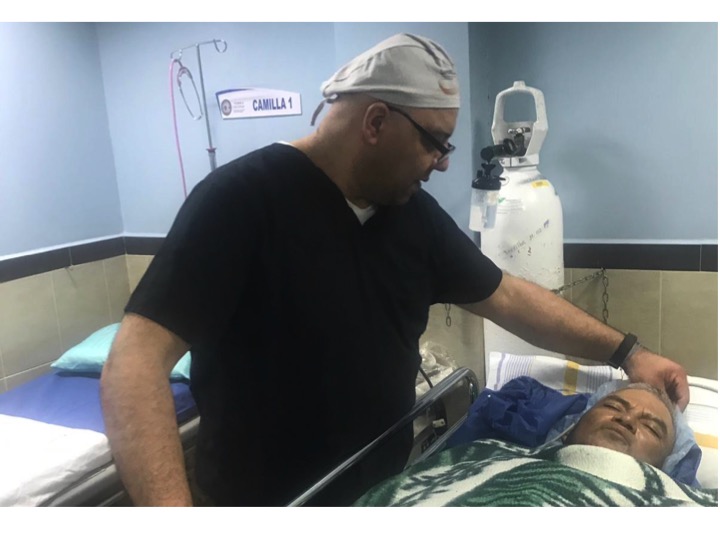
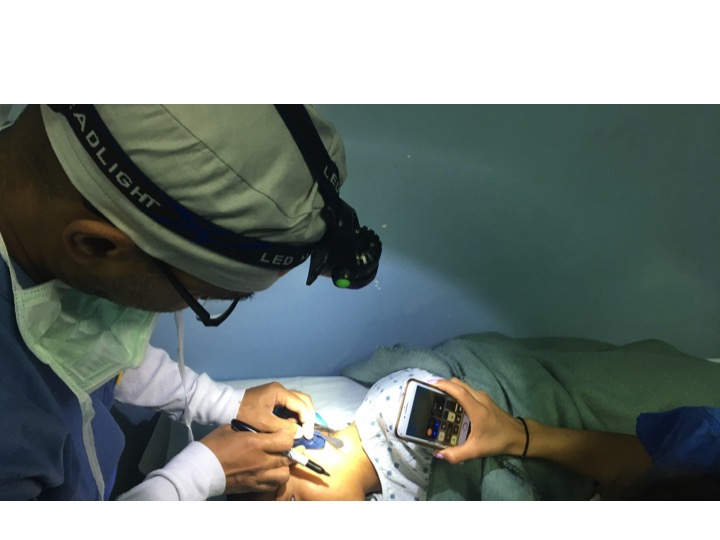
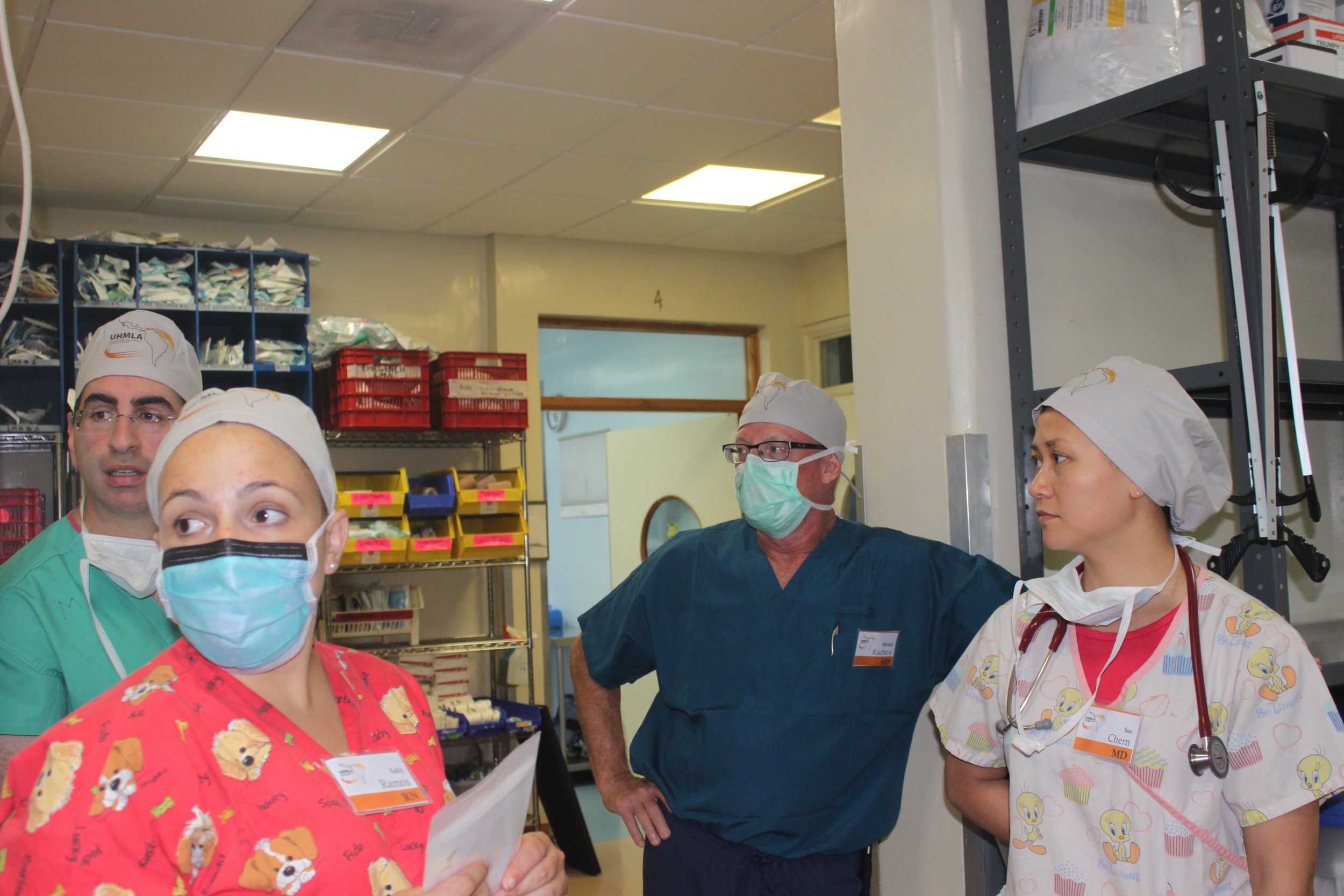
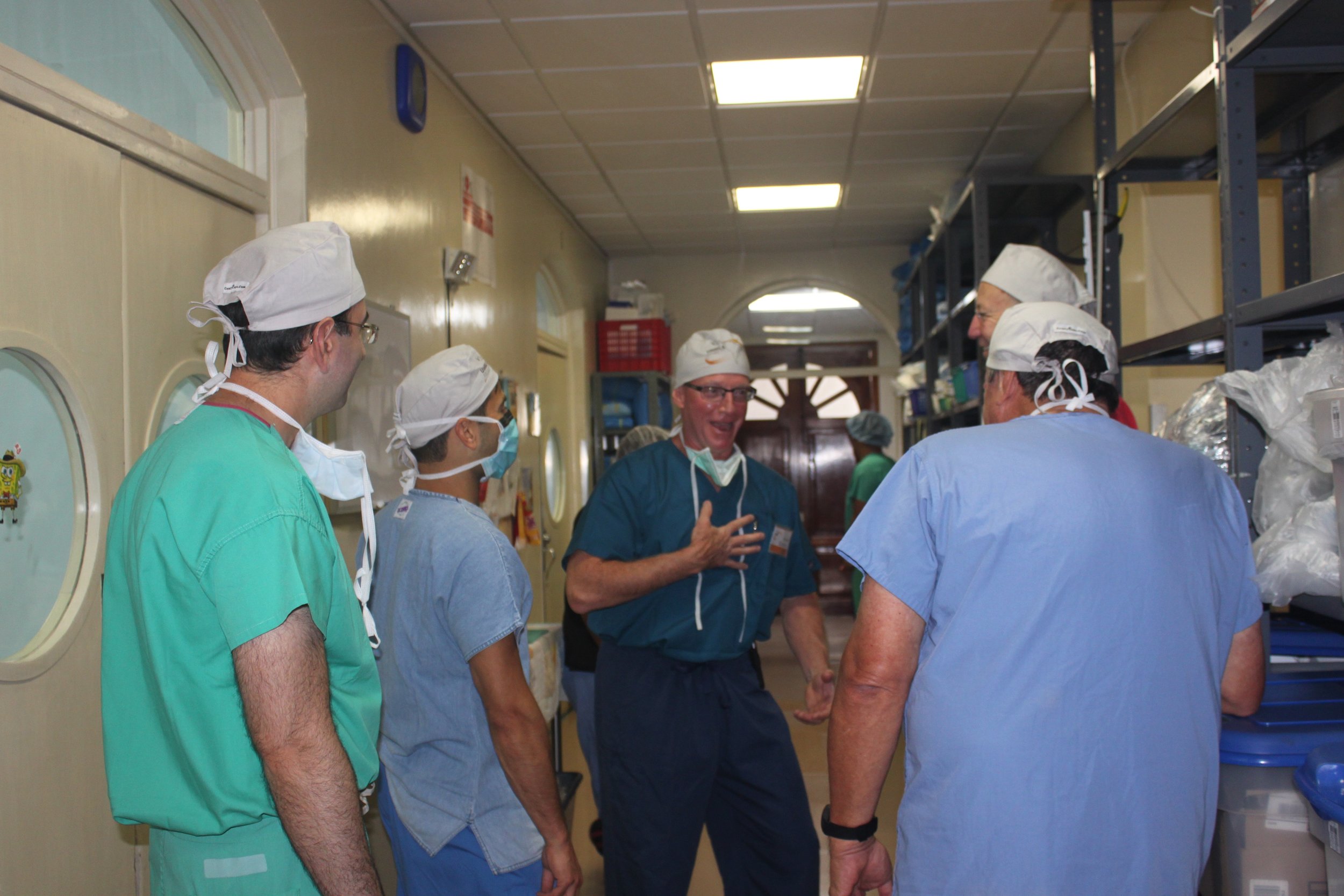
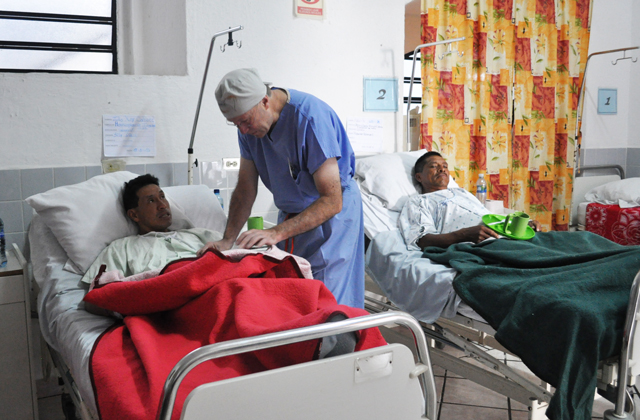
23 committed UHMLA members left on their mission trip on 10/13/2023 and returned home on 10/22/2023. From the start, the team meticulously organized their plan for the entire week, each day filled with long hours of tireless hard work. The initial day at the Clinic always holds particular significance as it involves crucial preparation work.The team begins their work by examining patients and selecting those most suitable for surgery. Some patients are happily released because surgery is not indicated, and they receive valuable medical advice. Unfortunately, some patients are rejected with a heavy heart due to complex diagnoses, and despite our desire to assist, our resources are not sufficient for a sustainable long-term treatment.
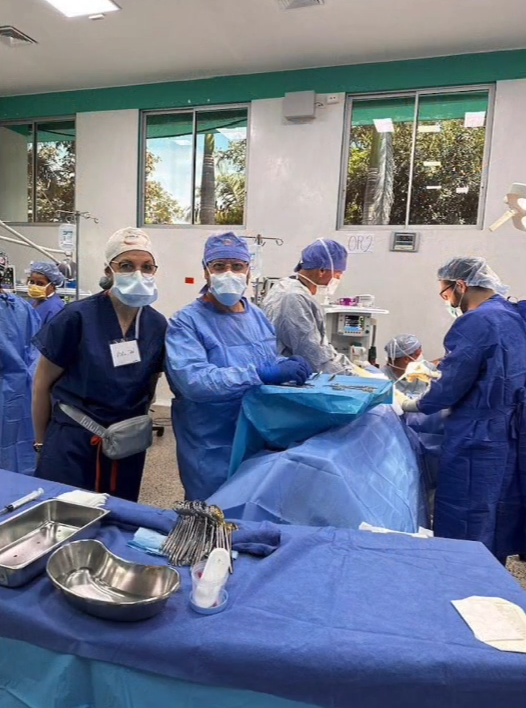
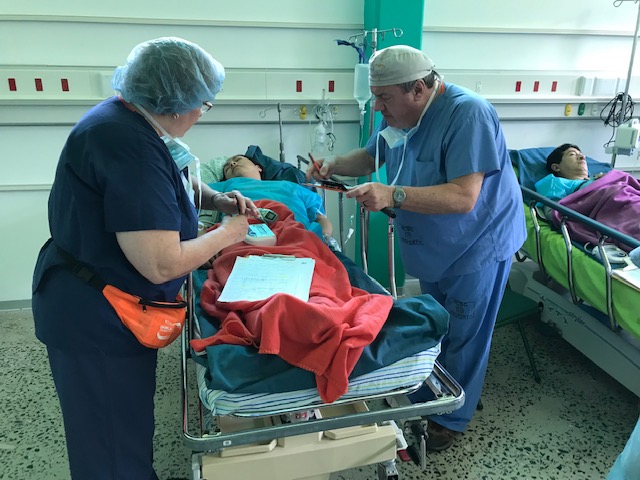
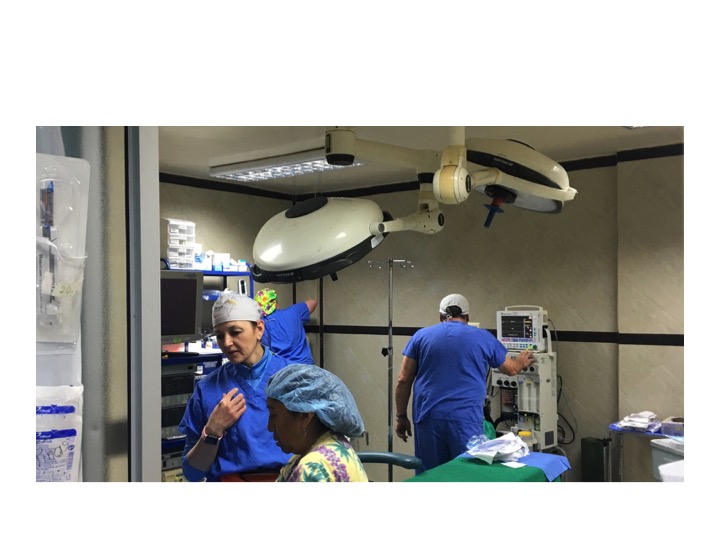
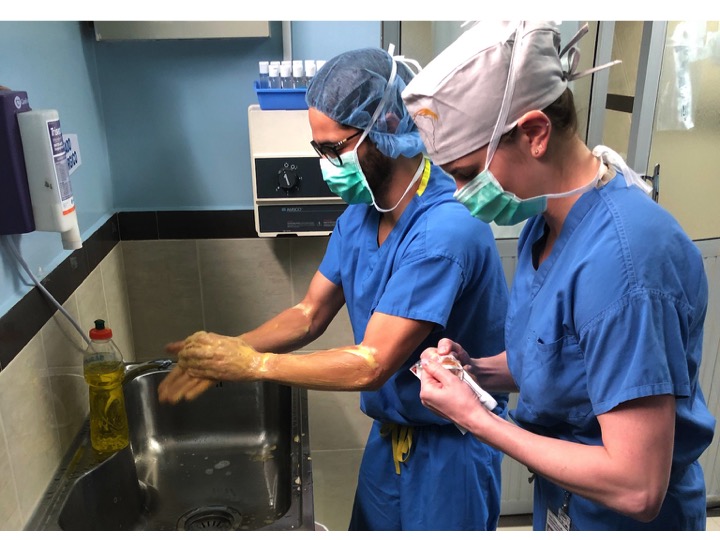
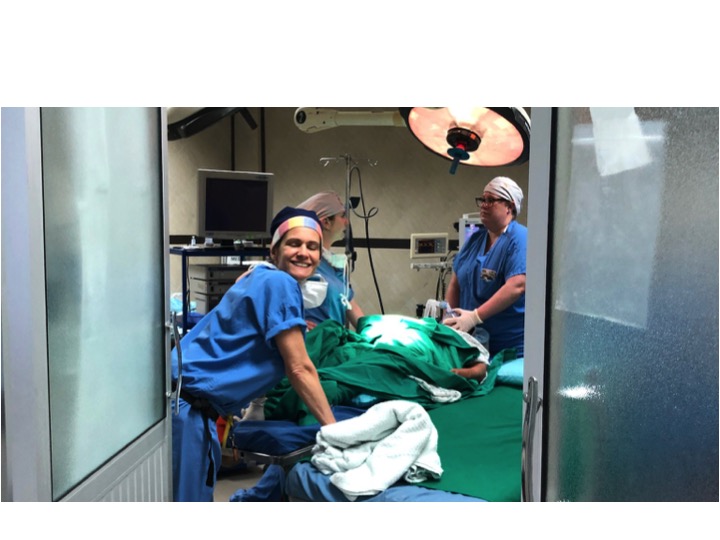
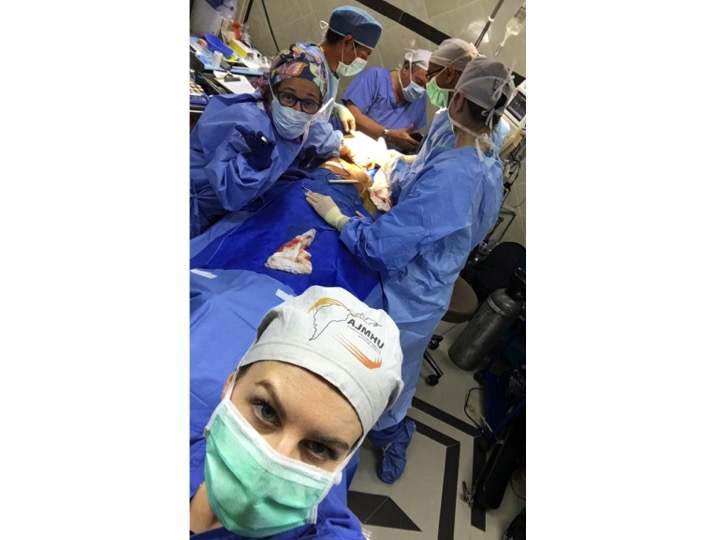
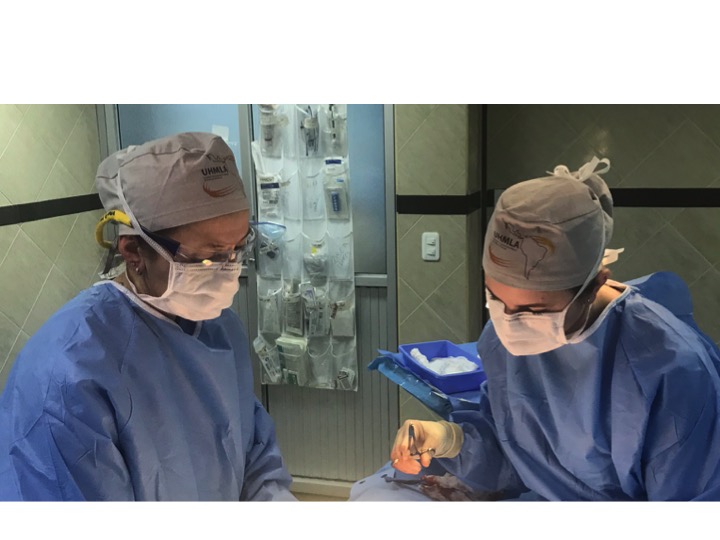
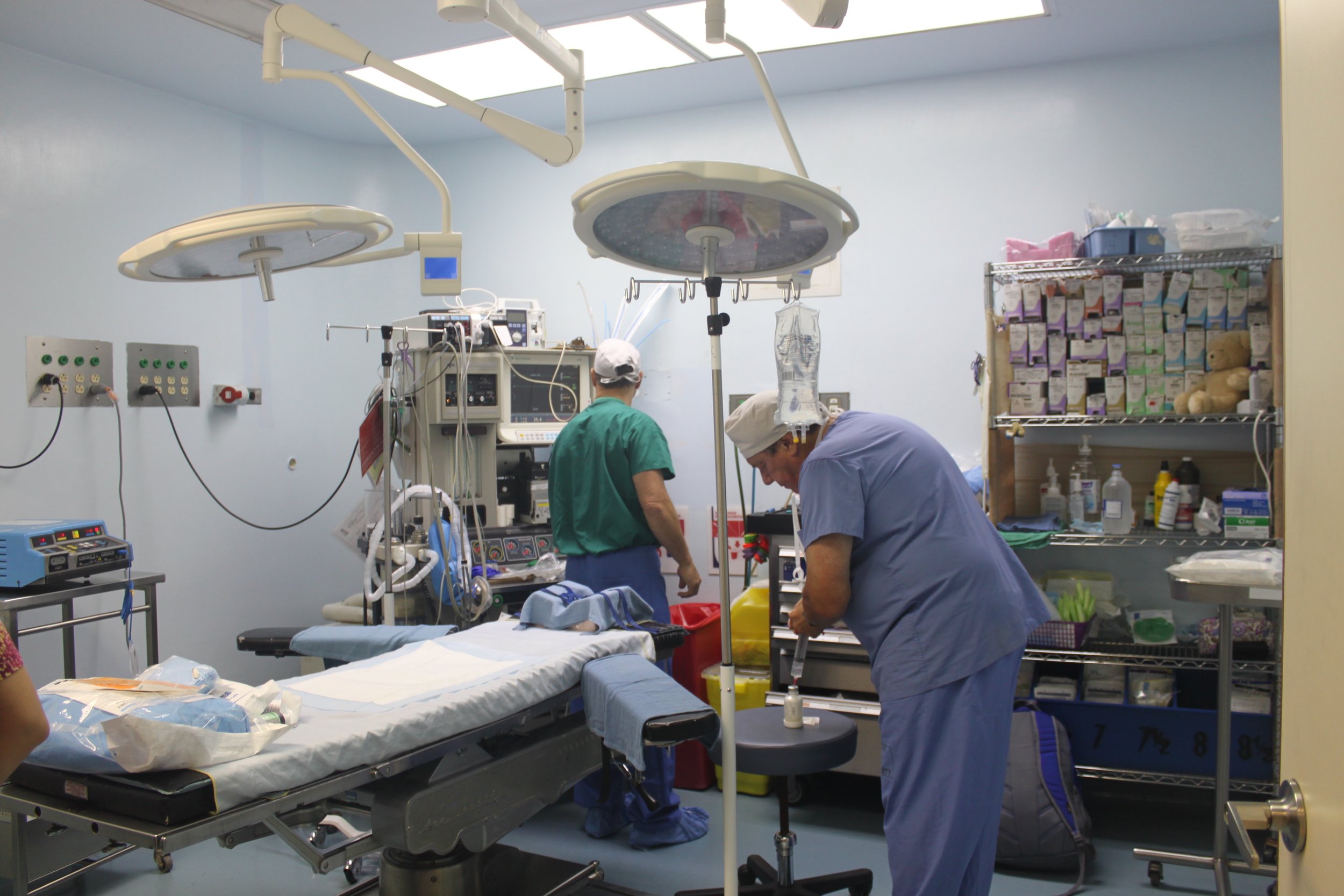
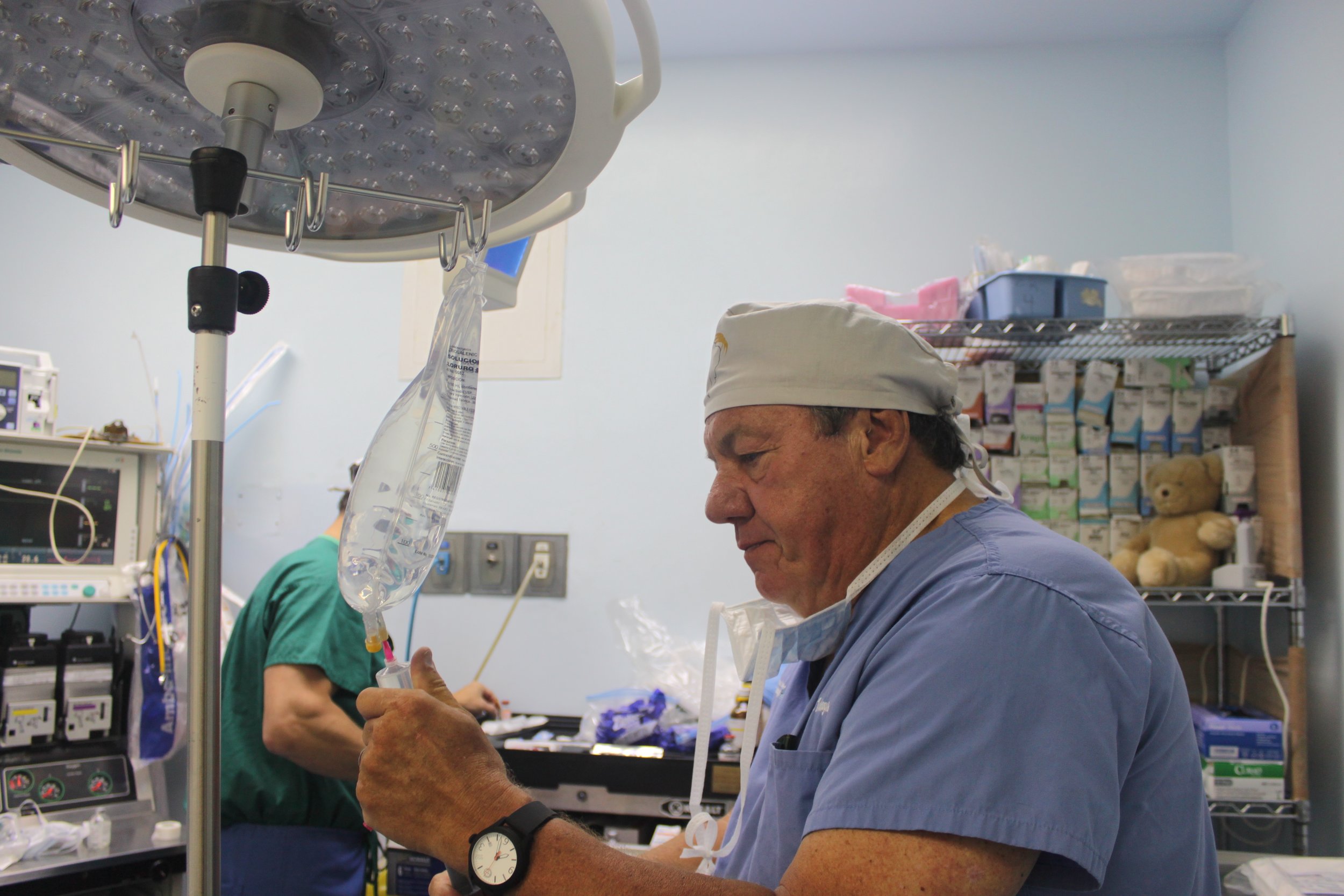
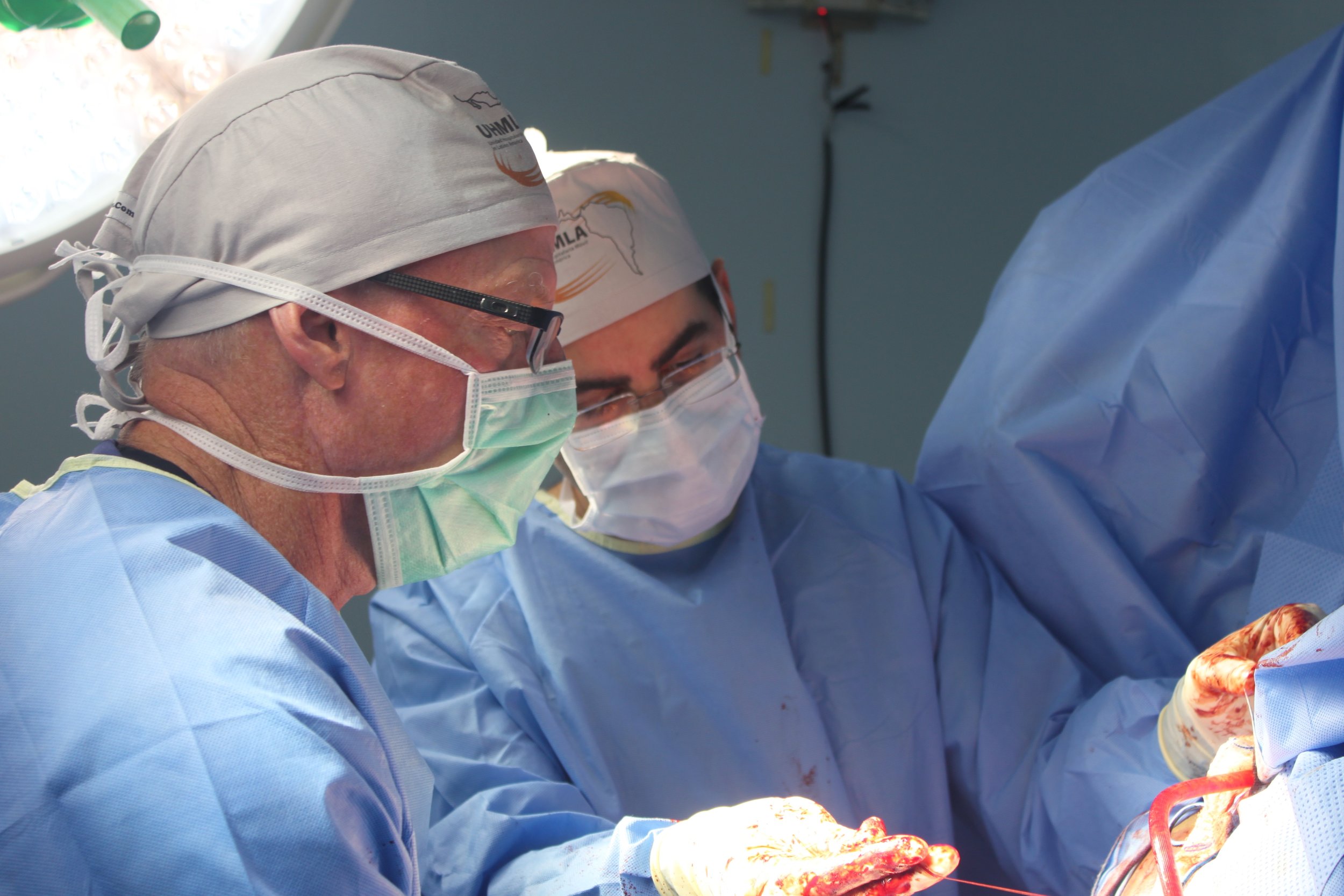
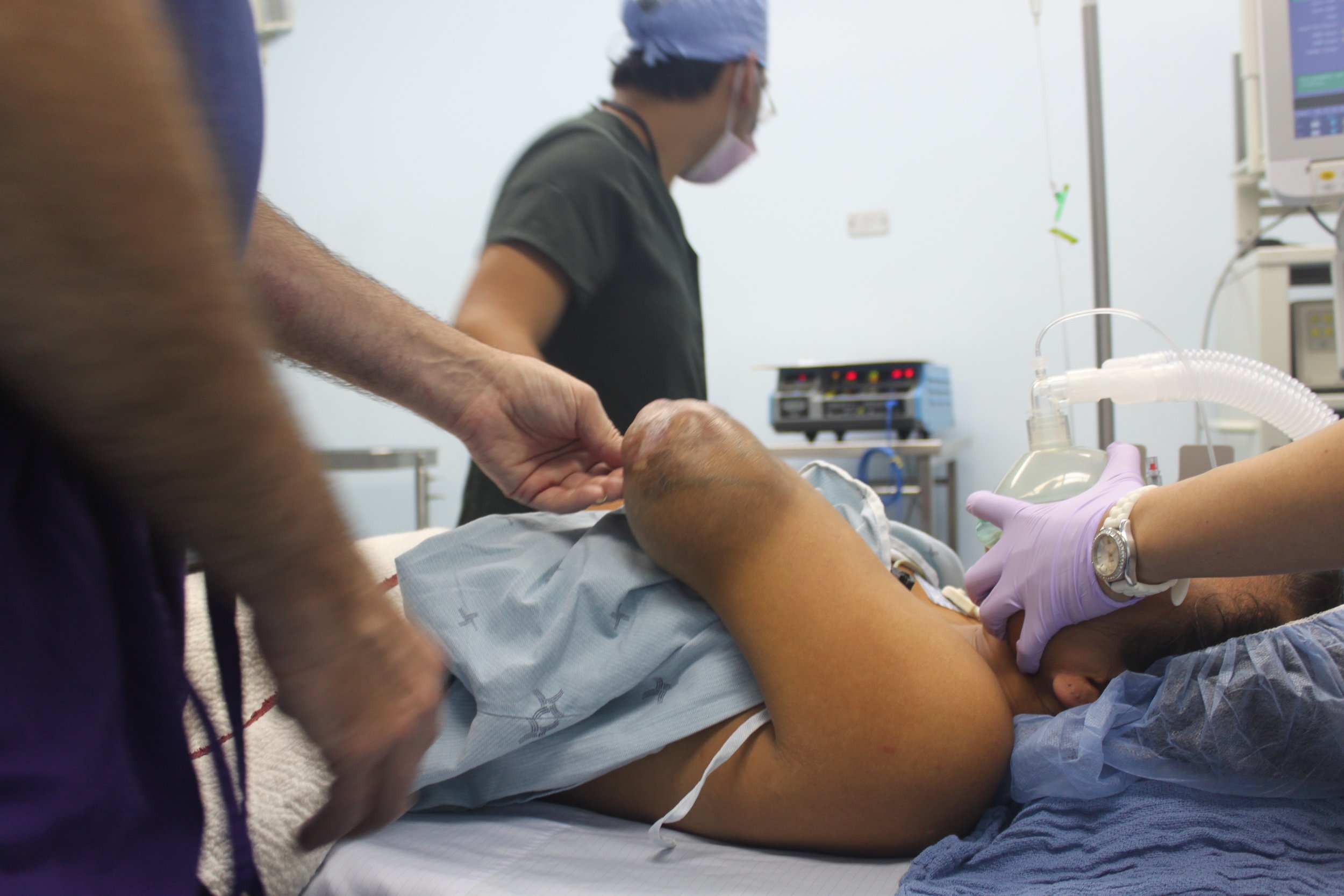
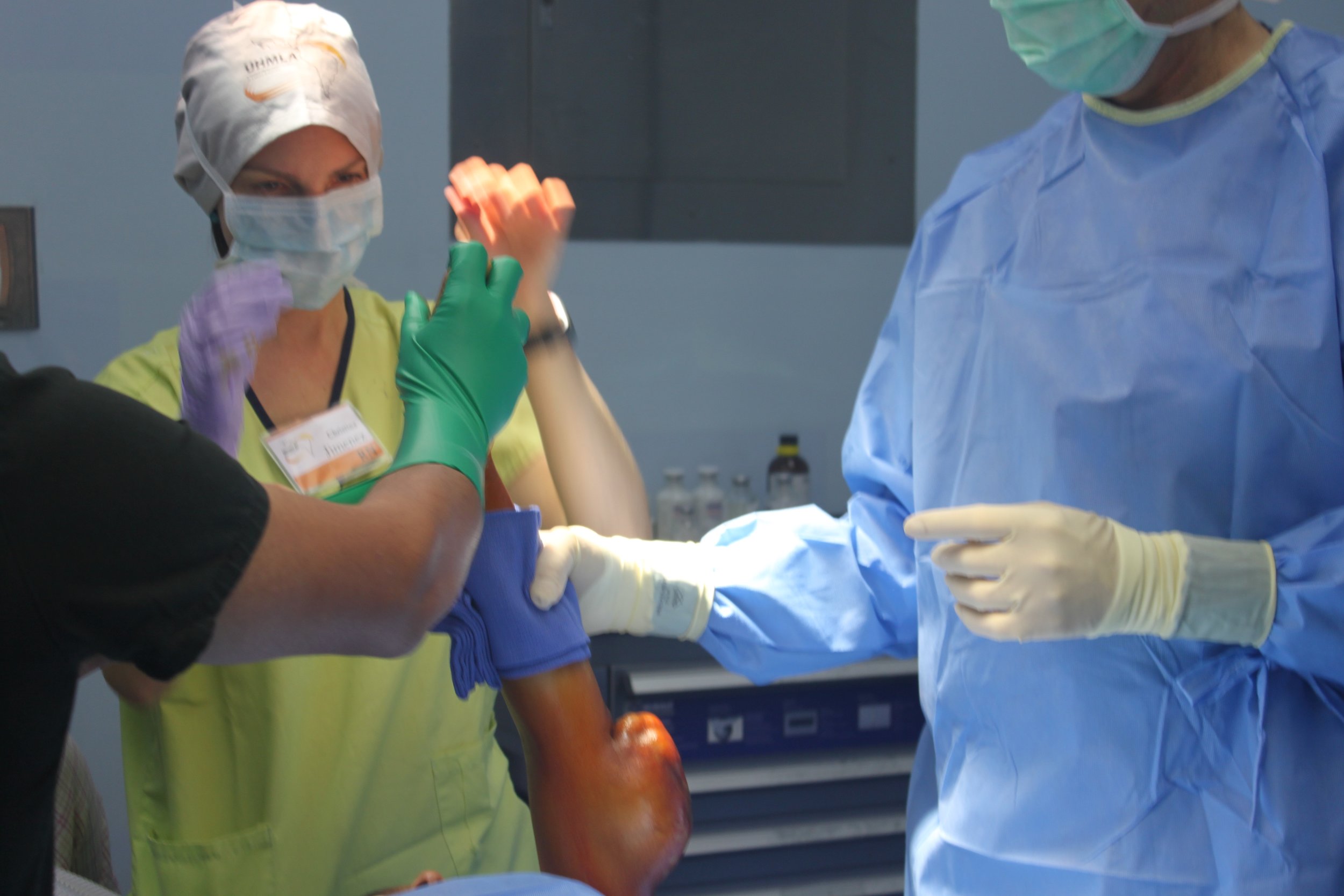
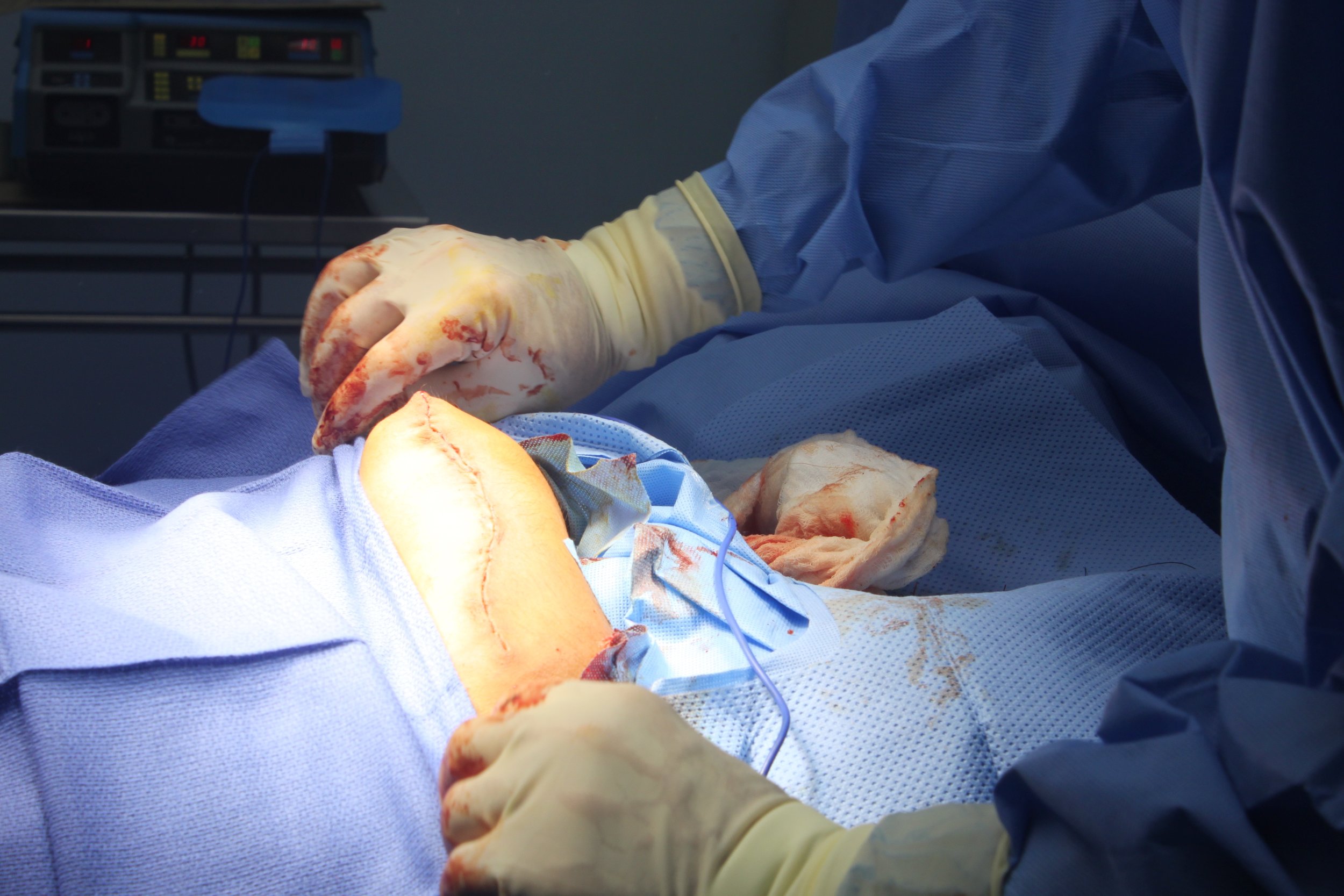
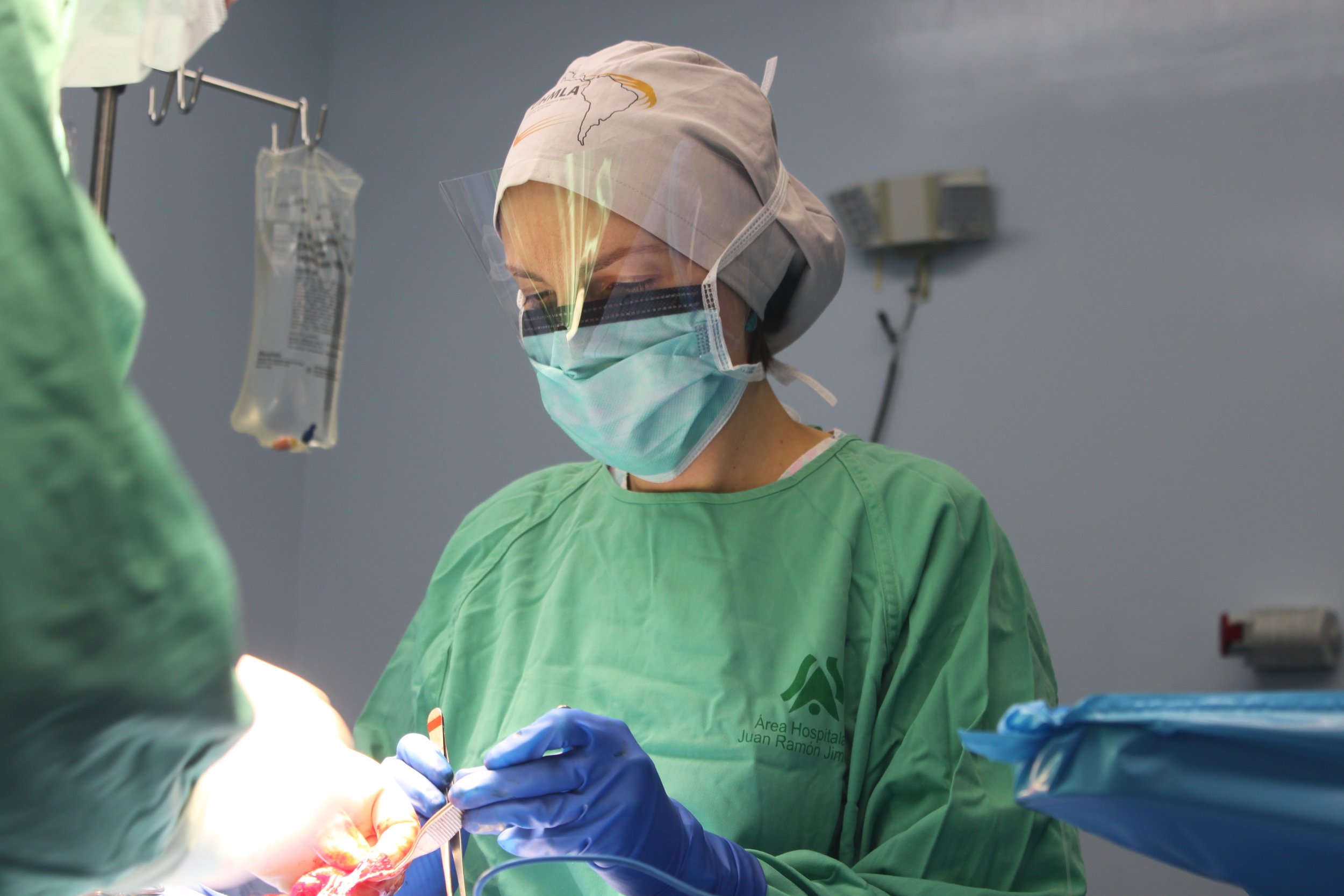
The first day is dedicated to organizing and staging supplies, sanitizing the entire peri-operative area, and finalizing the weekly surgery schedule. Following this extensive preparation, the team rolls up their sleeves even further, diving into performing surgeries and providing perioperative care with passion and dedication while ensuring the well-being of each patient.
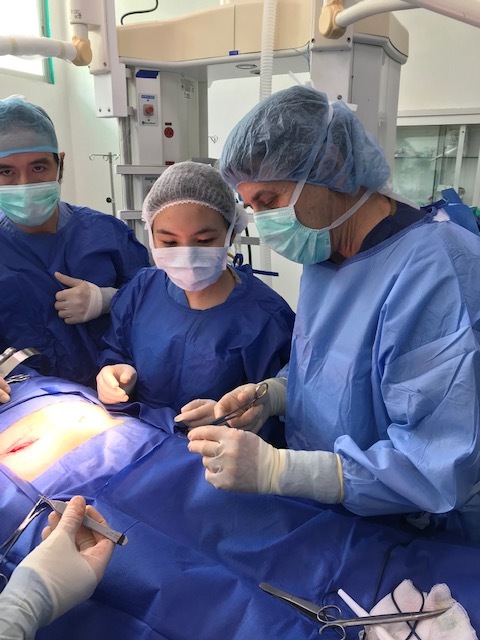
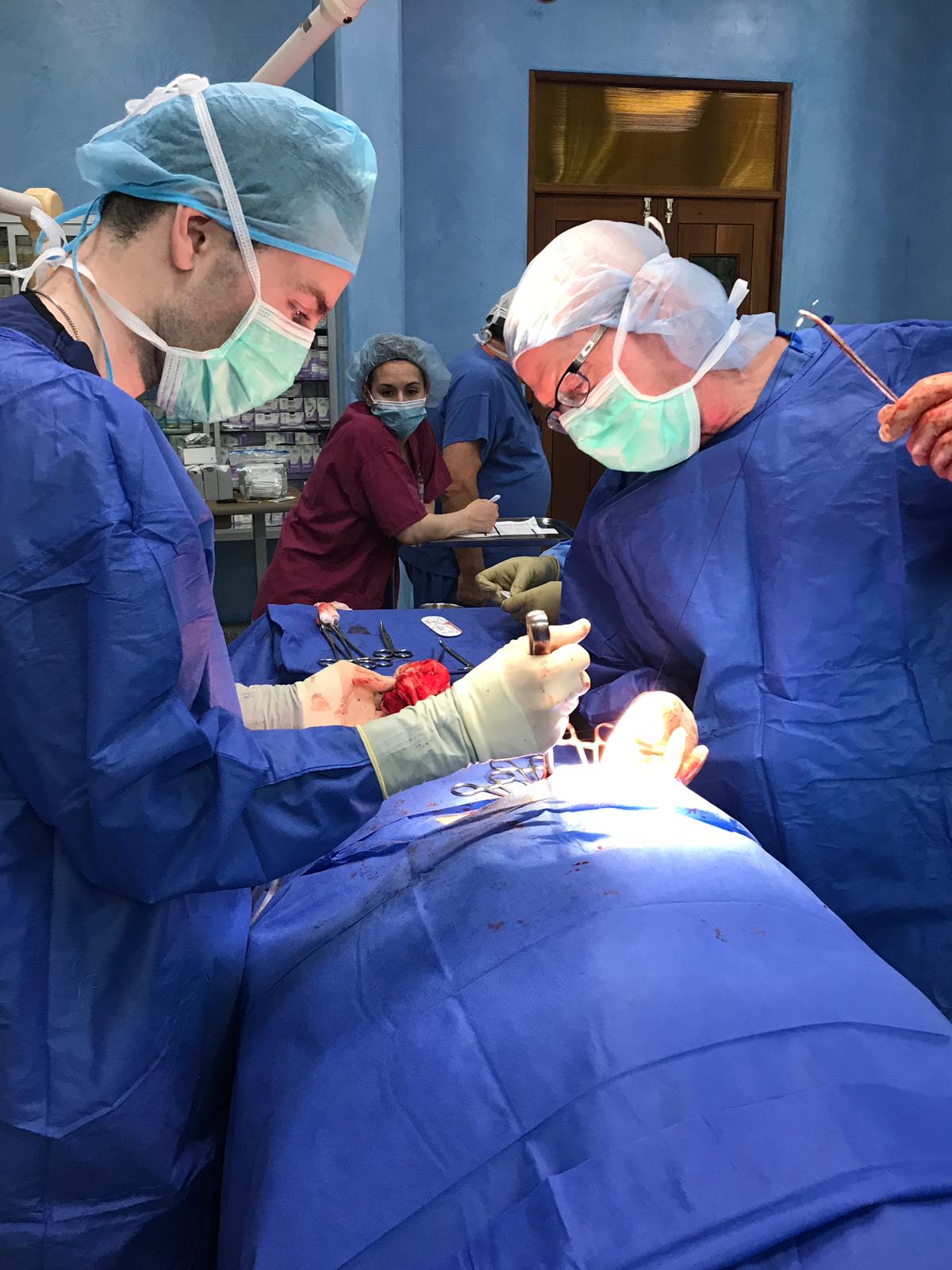
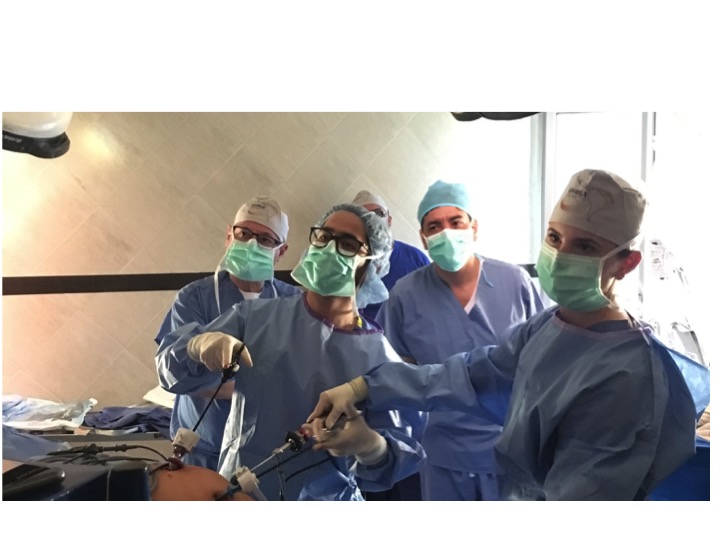
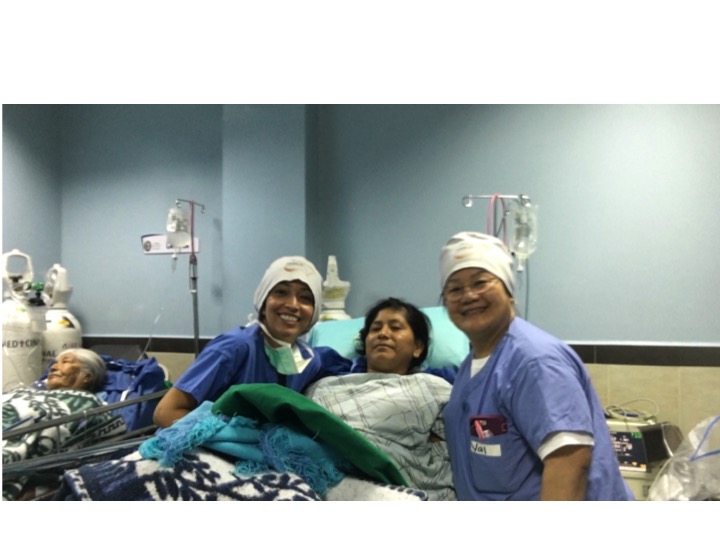
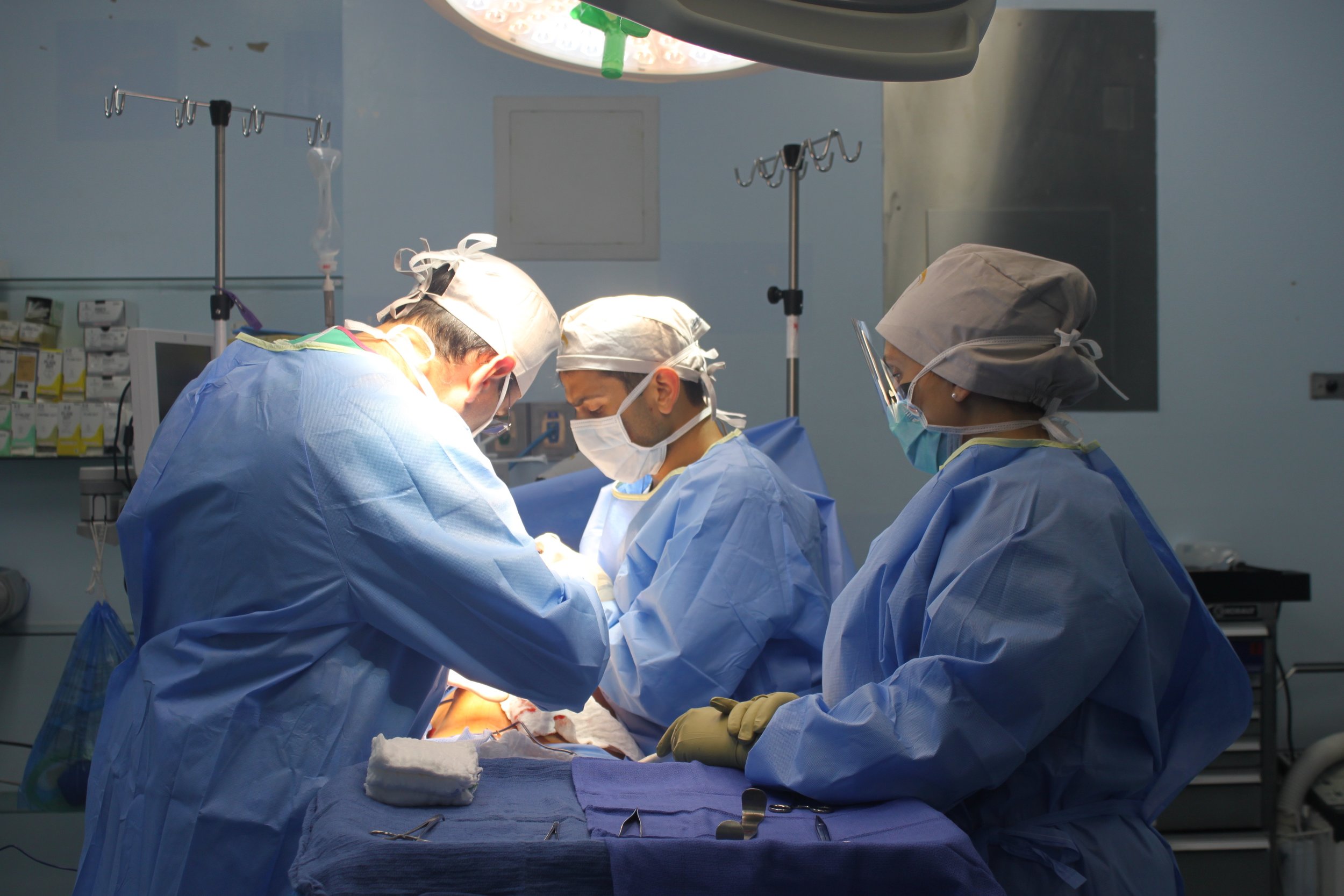
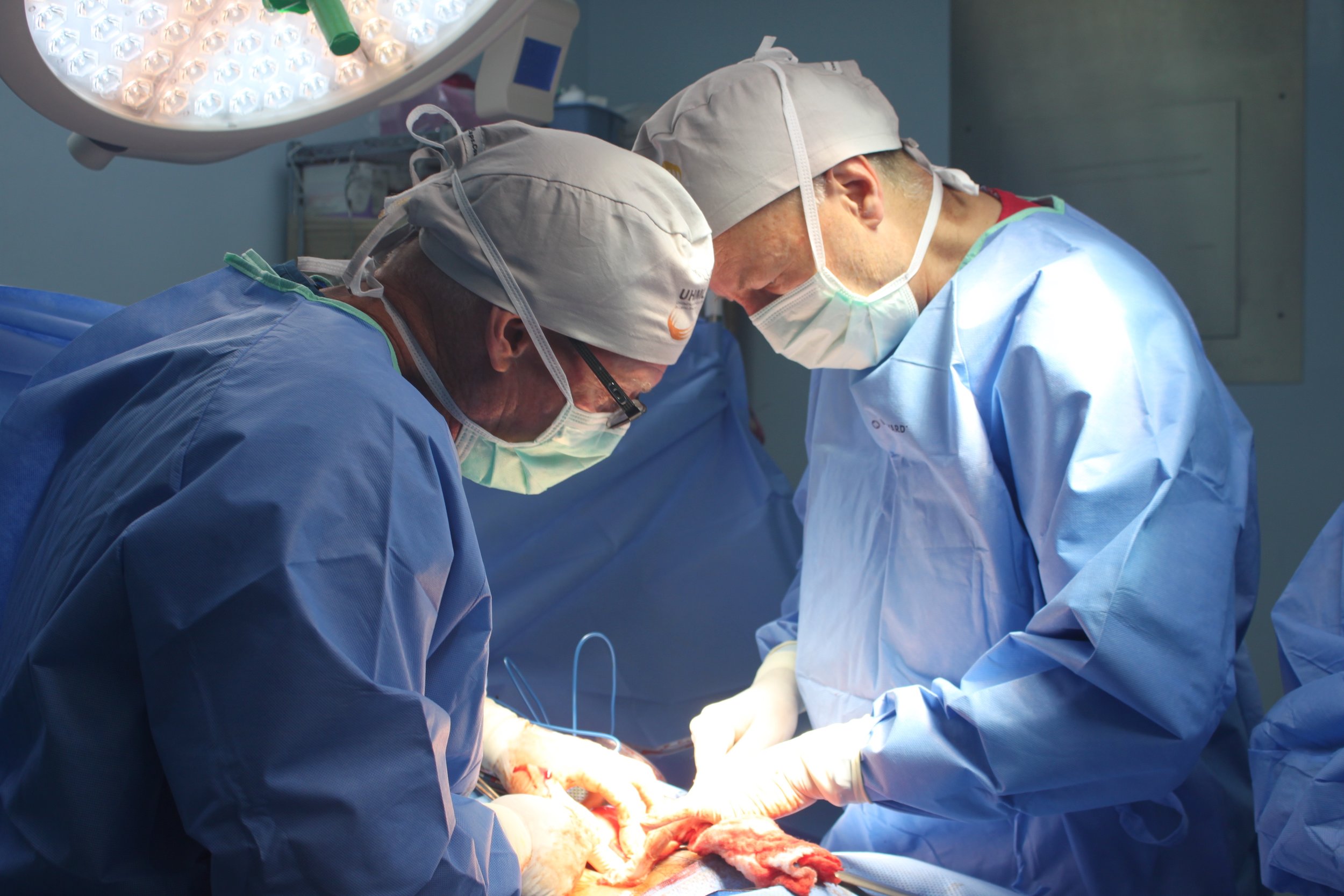
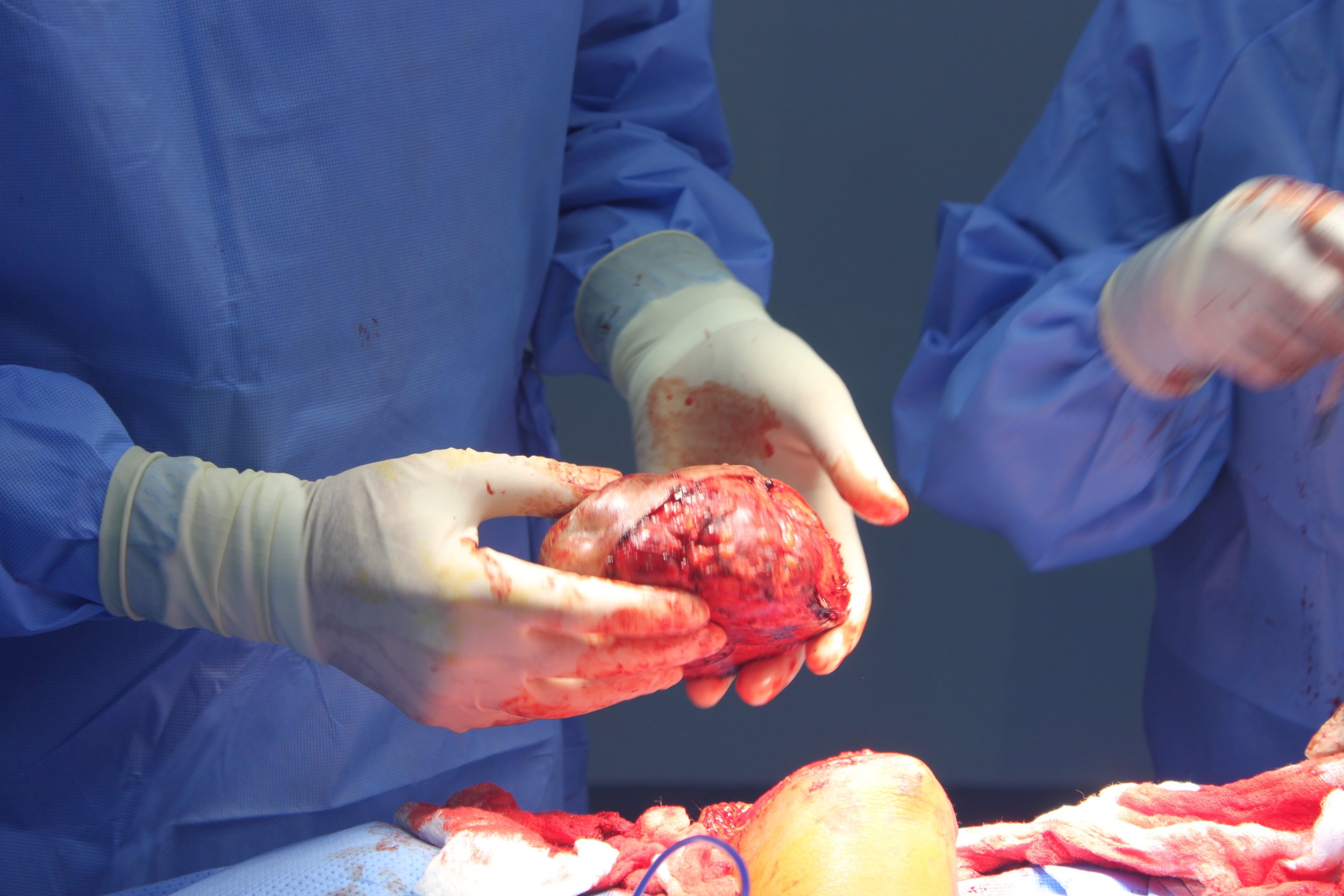
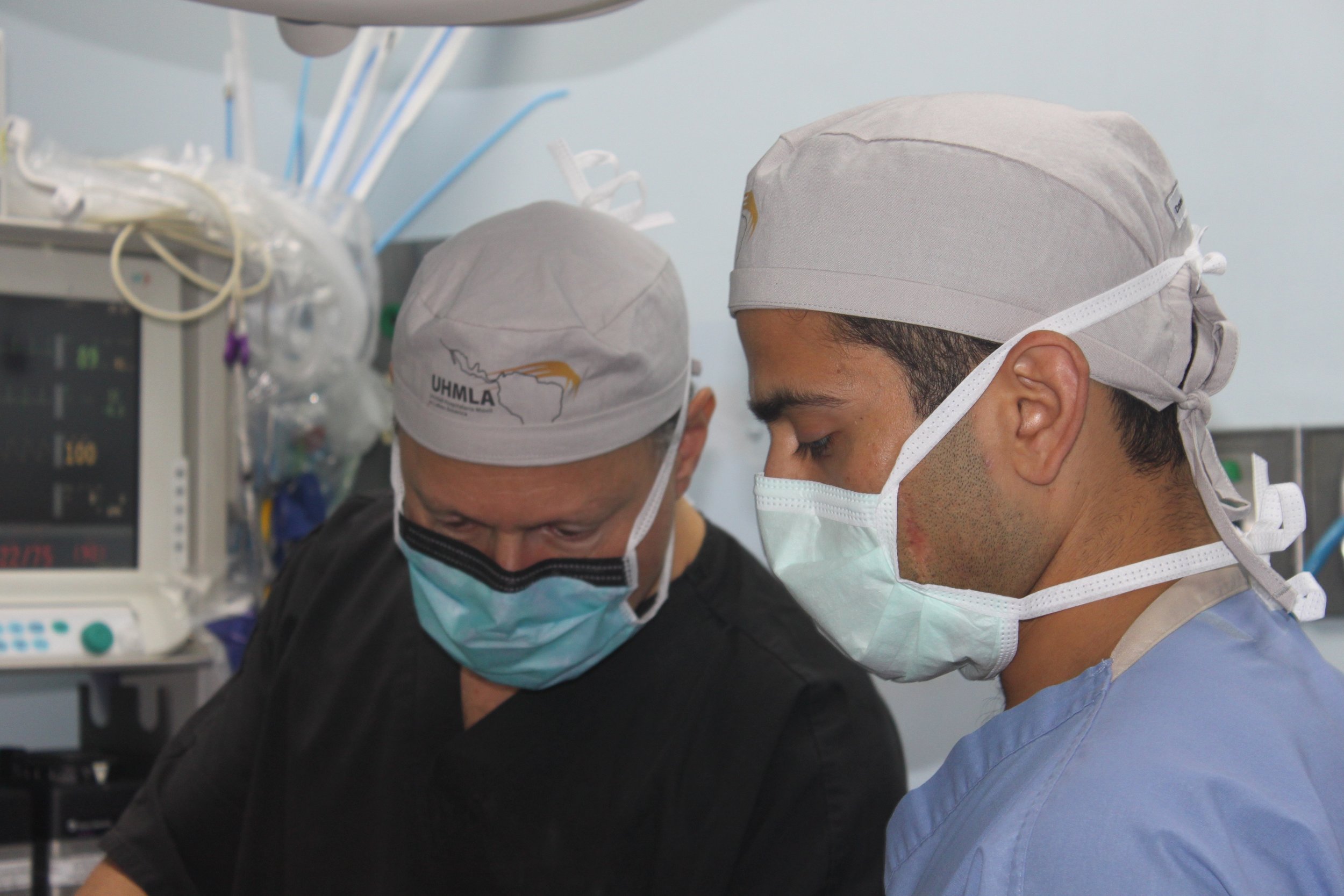
During this impactful trip UHMLA provided care to 59 patients through a range of surgeries, including gallbladder removal, hernia repair, excision of lipoma, breast lumpectomy, mastectomy, hysterectomy, vaginal prolapse procedures, and rectal procedures. Dr. William Diehl served as our surgeon leader, with Dr. Ricardo Caraballo and Dr. Anastasiya Holubyeva handling UROGYN procedures. Leading the general surgery team were Dr. Omar Ahmed, along with residents Dr. Anup Parikh and Dr. Sia Bolourani.
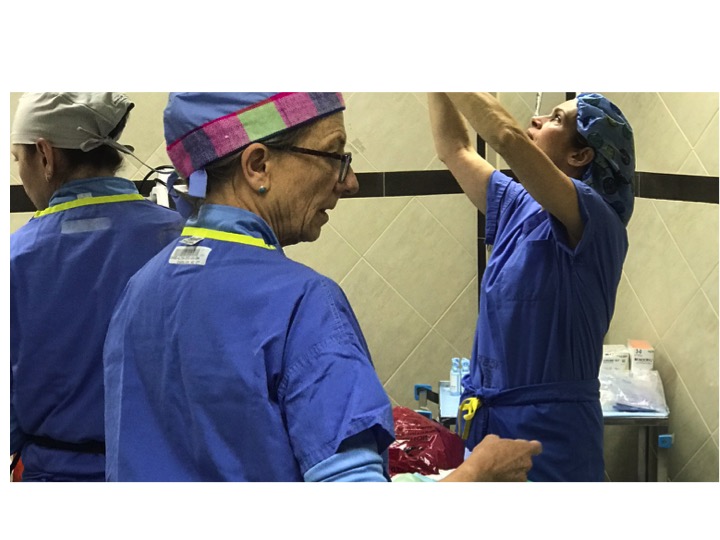
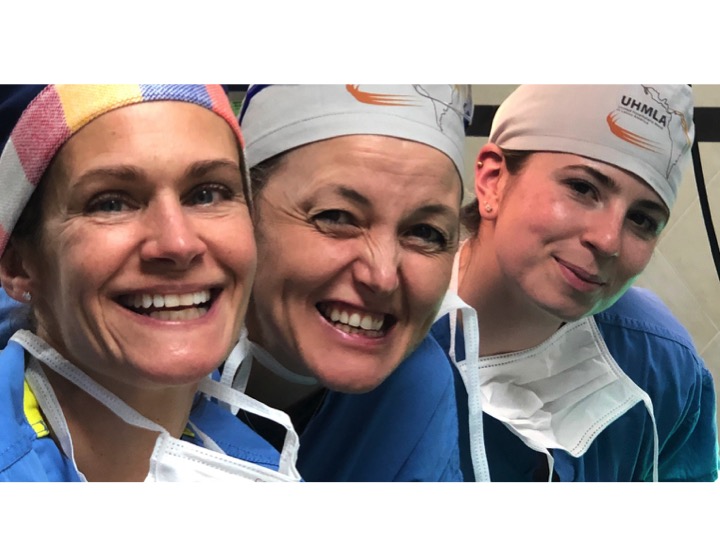
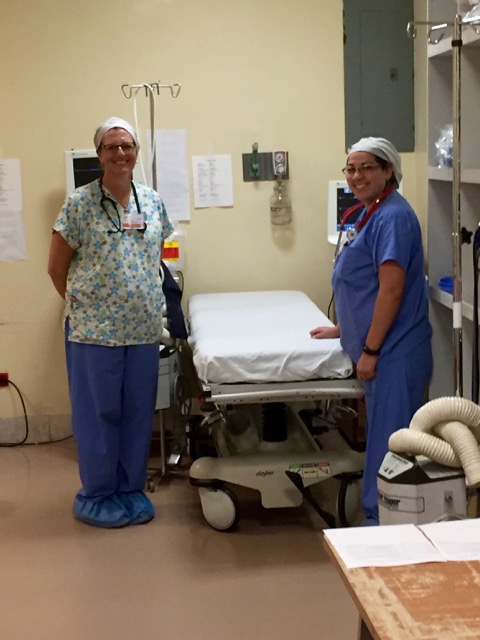
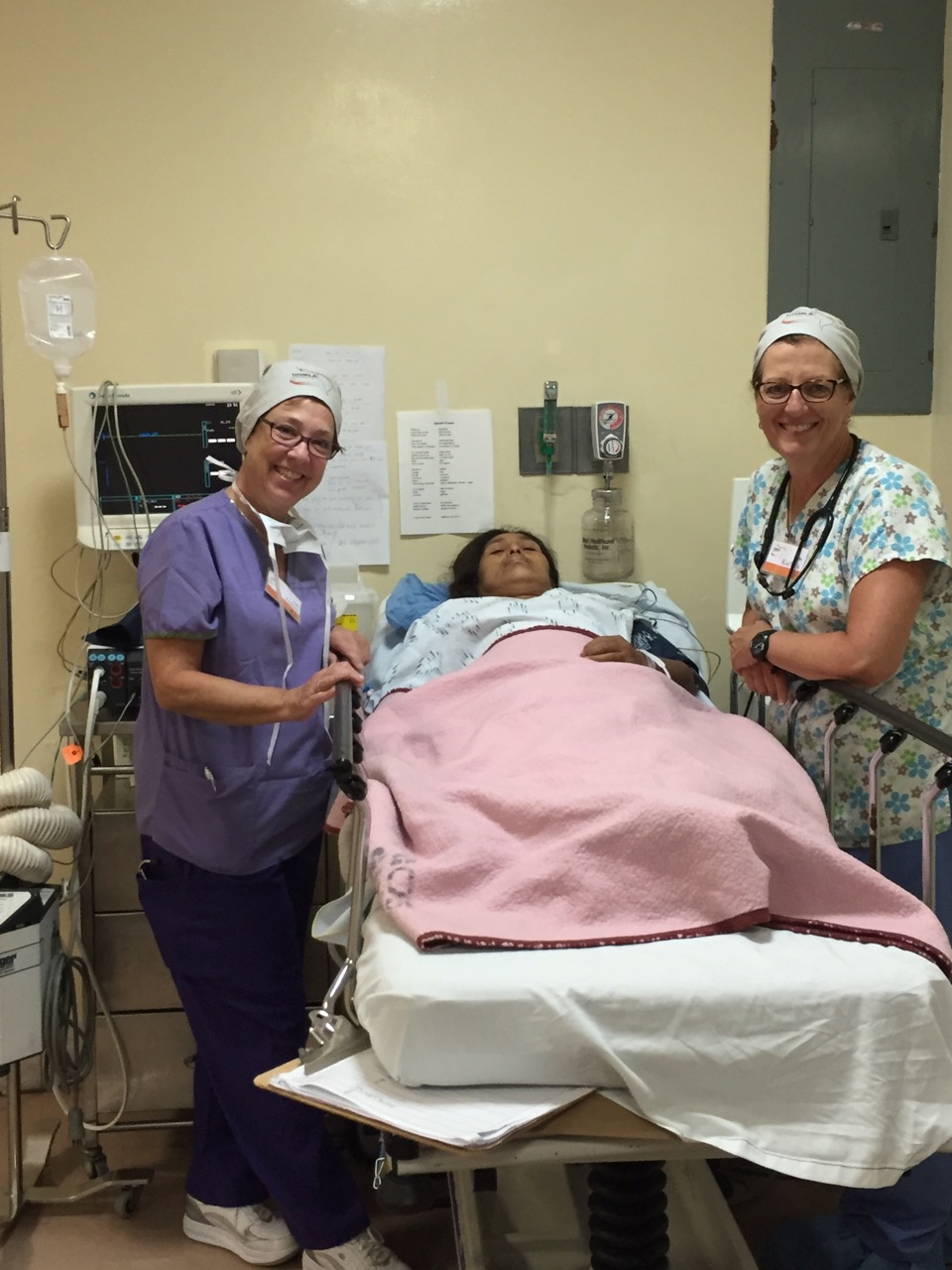
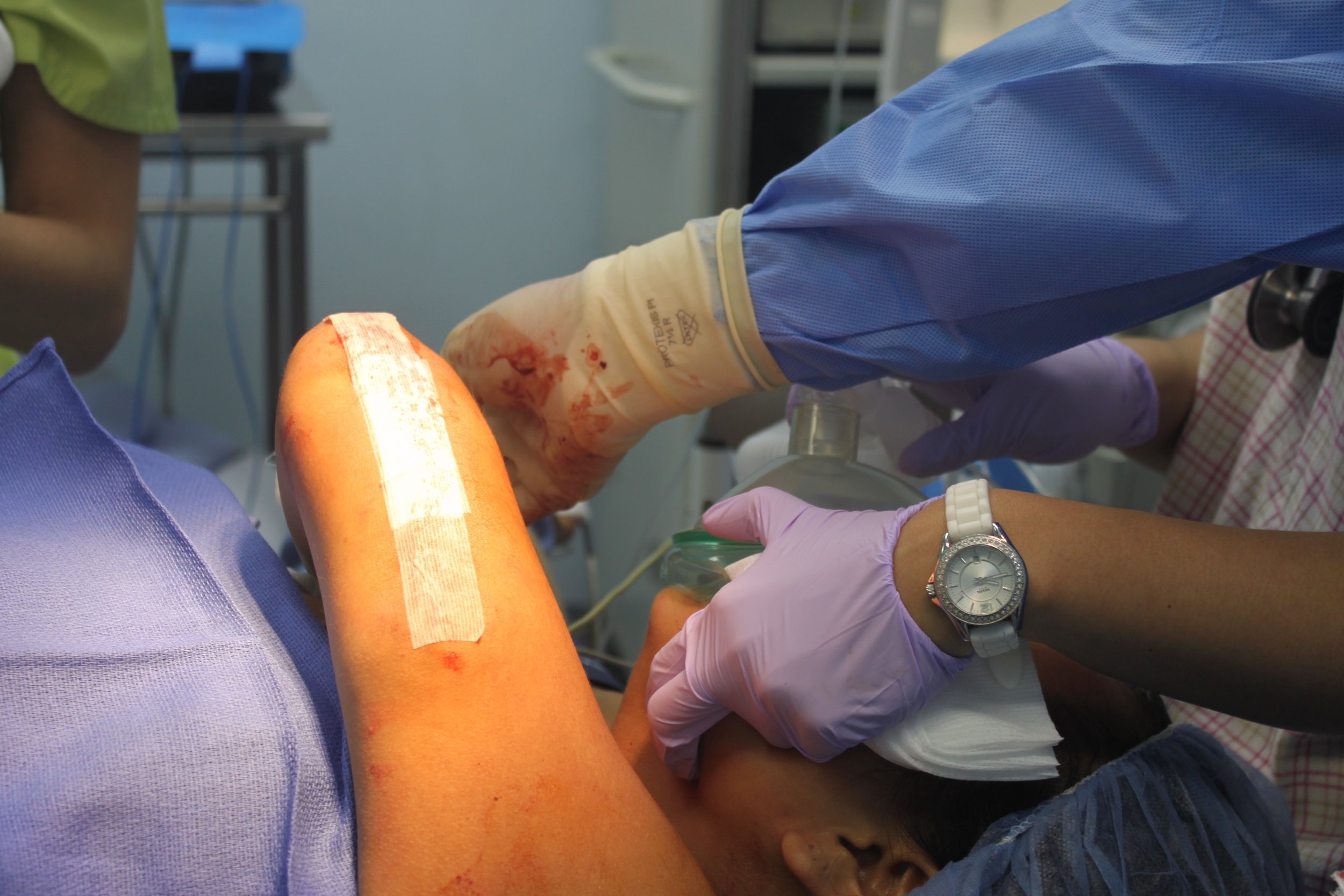
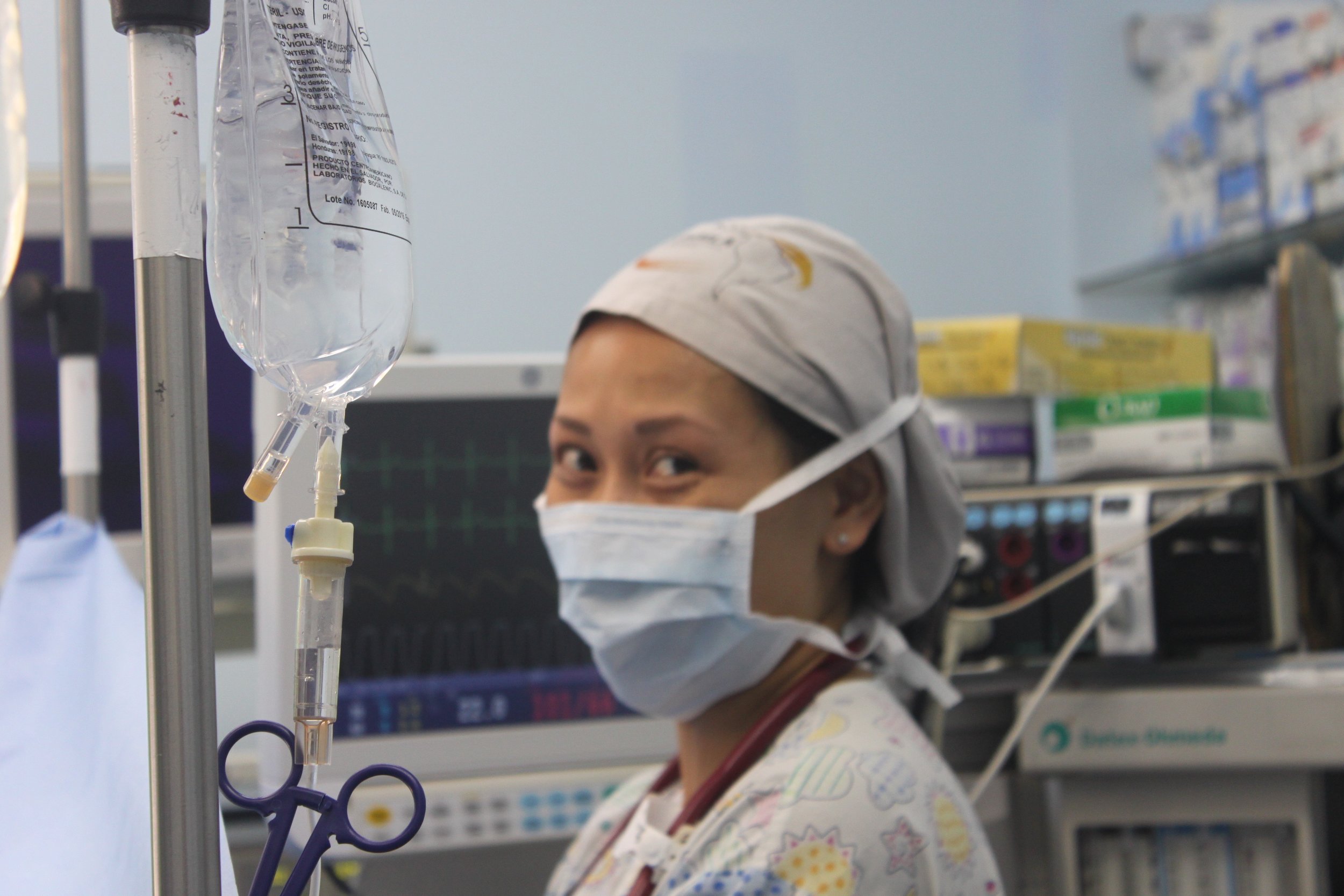
Our anesthesia team, comprising Dr. Jim Mattie, Dr. Igor Pikus, and CRNA Christina Brown, ensured the safety of our patients. In the Operating Room, the skilled nursing team included Maria Martinez, Olga Castro, Leslie Mongilia, Jim Pullara, Tara Gonzalez, and myself, Mel Ayhan. The PACU and Preop team, consisting of Rachel Thompson, Elizabeth Muchmore, Val Salvatore, and Judy Tracey, played crucial roles.
Surgical instrument handling was expertly managed by Jen Pagnillo, and Cicilia Gross provided much-needed support at multiple levels. Among these invaluable team members, Jen Pagnillo stood out as the MVP of the trip, recognized for her extraordinary efforts.
Similar to previous trips, this expedition also afforded participants life-changing experiences. Every member of this team underwent significant personal and professional growth, a rare opportunity to be found in the U.S. Each individual completed the trip with profound appreciation to UHMLA for the unique experience, leaving with feelings of gratitude and satisfaction and each team member expressed a sense of transformation, embodying a brand-new perspective.